Naturopathy for addiction recovery is gaining attention as more people look for safe, natural ways to overcome dependency. Addiction is not just a habit it affects the brain, body, and emotions deeply. Instead of relying only on medications, naturopathy focuses on healing the root cause through holistic methods like yoga, meditation, detoxification, and lifestyle changes. This approach works by restoring balance in the body, reducing cravings, and improving mental clarity over time. By combining natural therapies with mindful practices, individuals can regain control, rebuild healthier habits, and move toward long-term recovery in a more sustainable and supportive way.
What is Addiction?
Simple Definition of Addiction
Addiction is a chronic condition where a person repeatedly engages in a behavior or consumes a substance despite harmful consequences. It’s not about weak willpower or moral failure—it’s a complex brain disorder. Think of it as your brain’s reward system being hijacked. When you do something pleasurable, your brain releases dopamine, a feel-good chemical. In addiction, the brain learns to crave that activity or substance above all else, even when it causes problems with health, relationships, or finances.
Key point: Addiction is different from a bad habit. A habit you can usually break with effort; an addiction feels like you’ve lost control. Experts say addiction exists on a spectrum, from mild to severe, and it affects people from all walks of life.
How Addiction Affects the Brain
The brain has a built-in reward circuit designed to encourage survival behaviors like eating and social bonding. Addictive substances or behaviors flood this circuit with dopamine—sometimes two to ten times more than natural rewards. Over time, the brain adapts by producing less dopamine or reducing dopamine receptors. This means the person needs more of the substance or behavior just to feel “normal.”
Here’s what changes: The prefrontal cortex, responsible for decision-making and impulse control, becomes less active. Meanwhile, the amygdala, which handles stress and cravings, becomes more sensitive. Studies show these changes can persist long after someone stops using. That’s why triggers—like seeing a bar or feeling stressed—can spark intense cravings months or even years into recovery. Understanding this brain science helps replace shame with compassion.
Why Understanding Types of Addiction is Important
Impact on Physical Health
Different addictions damage the body in different ways, but all take a toll. Substance addictions can lead to liver disease, lung damage, heart problems, or neurological issues. Behavioral addictions—like gambling or gaming—often result in sleep deprivation, poor nutrition, and sedentary lifestyles. Even “hidden” addictions like compulsive shopping can cause stress-related physical symptoms such as headaches, high blood pressure, and digestive problems.
Recognizing the physical signs early—chronic fatigue, sudden weight changes, or frequent illnesses—can be a wake-up call. The body often signals trouble before the mind fully accepts there’s a problem.
Impact on Mental and Emotional Well-being
Addiction and mental health are deeply connected. Many people use substances or behaviors to self-medicate anxiety, depression, or past trauma. But over time, addiction worsens these very conditions. The cycle looks like this: temporary relief from a drink or a shopping spree, followed by guilt, shame, and deeper emotional pain. This leads back to the addictive behavior for escape.
Common emotional effects include: irritability, mood swings, low self-worth, and feelings of hopelessness. Anxiety disorders and depression are significantly more common among those with addiction. Understanding this link is crucial because treating only the addiction without addressing underlying emotional wounds often leads to relapse.
Hidden Addictions in Daily Life
Not all addictions look dramatic or obvious. Hidden addictions—sometimes called “socially acceptable” addictions—fly under the radar because they don’t cause obvious intoxication or financial ruin overnight. These include compulsive use of social media, online shopping, work, exercise, or even romantic relationships.
A person might spend four hours nightly scrolling through apps, neglecting sleep and family time, yet insist “it’s not a real addiction.” Experts say any behavior that feels compulsive, causes distress when stopped, and negatively impacts daily functioning qualifies as problematic. Recognizing these hidden patterns is the first step toward change, because they’re often the very behaviors we dismiss as “just how everyone lives now.”
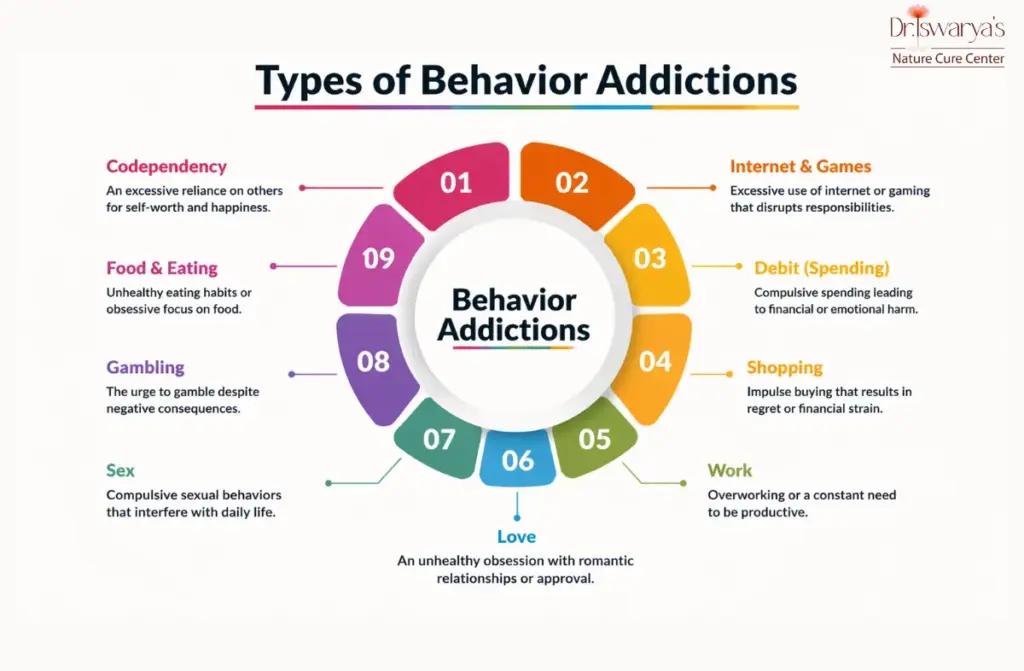
Main Types of Addiction
Substance Addiction
This is the most widely recognized form. Substance addiction involves the compulsive use of chemicals that alter brain function. Common examples include:
- Alcohol – Legal but potentially devastating
- Nicotine – Highly addictive, found in tobacco and vapes
- Prescription drugs – Opioids, benzodiazepines, and stimulants
- Illegal drugs – Cocaine, heroin, methamphetamine, cannabis
Withdrawal symptoms vary by substance but often include nausea, shaking, anxiety, and intense cravings. Substance addiction can develop quickly or over years, and it doesn’t discriminate by age, income, or background.
Behavioral Addiction
Here, the addiction isn’t to a chemical but to an activity that triggers the brain’s reward system. Gambling disorder is the most researched behavioral addiction, recognized in medical diagnostic manuals. Others include:
- Gaming addiction – Especially online multiplayer games
- Pornography addiction – Compulsive viewing despite negative consequences
- Shopping addiction – Buying items for the rush, not the need
- Sex addiction – Compulsive sexual thoughts or acts
These addictions often go unnoticed because there’s no visible substance involved. But the brain changes—dopamine dysregulation, craving cycles, loss of control—are remarkably similar to substance addiction.
Lifestyle and Habit Addiction
These are repetitive daily behaviors that become compulsive and hard to break. While less severe than clinical addiction, they still reduce quality of life. Examples include:
- Caffeine addiction – Inability to function without multiple cups of coffee
- Sugar addiction – Craving sweets even when full or experiencing health issues
- Internet/smartphone addiction – Constant checking, fear of missing out
- Workaholism – Compulsive overworking that harms health and relationships
The line between a strong habit and addiction is whether you can stop without significant distress or withdrawal symptoms. For many people, these lifestyle addictions serve as coping mechanisms for boredom, stress, or loneliness.
Psychological and Emotional Addiction
This type focuses less on a specific substance or activity and more on an emotional state. People become “addicted” to certain feelings, such as:
- Adrenaline addiction – Seeking danger or chaos for the rush
- Romance/relationship addiction – Jumping from intense relationship to relationship
- Validation addiction – Needing constant approval from others (social media likes, compliments)
- Misery addiction – Unconsciously staying in negative thought patterns because they feel familiar
Psychological addictions often stem from childhood experiences or trauma. A person might not realize they’re addicted to drama until they notice every calm relationship feels “boring” or every peaceful moment brings discomfort.
Positive or “Good” Addictions
Yes, some addictions can be constructive—though experts debate whether to call them “addictions” at all. The term is sometimes used for healthy habits that people feel driven to do daily. Examples include:
- Exercise addiction – When balanced, it’s healthy; when compulsive (even while injured), it’s problematic
- Learning addiction – Constantly seeking new knowledge
- Meditation or spiritual practice – Feeling “off” without daily practice
The difference between positive and negative addiction lies in consequences. A positive habit enhances life without harm. If exercise causes injuries or missed work, or meditation becomes an escape from real problems, it may have crossed a line. Still, channeling addictive tendencies into beneficial activities can be a recovery strategy.
Common Signs and Symptoms of Addiction
Physical Signs
The body often shows the earliest clues. Physical signs vary depending on the addiction but commonly include:
- Changes in sleep patterns – Insomnia or sleeping excessively
- Appetite or weight changes – Sudden gain or loss
- Bloodshot eyes or dilated pupils
- Poor hygiene or unkempt appearance
- Frequent illness – Weakened immune system
- Tremors or slurred speech (with alcohol or certain drugs)
- Unexplained injuries (accidents during intoxication)
For behavioral addictions, physical signs might include headaches from screen time, back pain from prolonged sitting, or exhaustion from late-night gaming sessions.
Behavioral Changes
Behavioral signs are often what loved ones notice first. These include:
- Secrecy – Lying about activities or hiding evidence
- Loss of control – Using more than intended or for longer periods
- Failed attempts to quit – Multiple promises to stop that don’t last
- Neglecting responsibilities – Missing work, school, or family events
- Risky behavior – Driving drunk, unsafe sex, financial gambles
- Loss of interest – Abandoning hobbies and friendships once enjoyed
A person might also develop rituals around their addiction—needing to gamble before work, drink only at certain times, or check their phone every few minutes.
Emotional Symptoms
Inside, someone struggling with addiction often experiences a storm of emotions:
- Irritability and agitation – Especially when unable to engage in the behavior
- Anxiety – Worrying about getting the next “fix” or hiding the problem
- Depression – Feeling hopeless or worthless
- Guilt and shame – Knowing the behavior is harmful but feeling unable to stop
- Defensiveness – Getting angry when anyone suggests a problem
- Emotional numbness – Feeling disconnected from normal joys and sorrows
These emotional symptoms often worsen over time, creating a vicious cycle where the person uses the addiction to escape the very feelings the addiction caused.
Causes of Addiction
Stress and Mental Health Issues
Stress is one of the most powerful drivers of addiction. When life feels overwhelming—whether from work pressure, financial problems, or relationship conflicts—people naturally seek relief. A drink, a shopping spree, or hours of gaming provides temporary escape. Over time, the brain learns that this behavior reduces stress, making it the go-to coping mechanism.
Mental health conditions strongly linked to addiction include: depression, anxiety disorders, PTSD, bipolar disorder, and ADHD. Experts call this “dual diagnosis” or co-occurring disorders. Often, the addiction starts as self-medication. Someone with social anxiety might drink to feel comfortable at parties. A person with PTSD might use marijuana to suppress nightmares. Without treating the underlying condition, lasting recovery is extremely difficult.
Genetic and Biological Factors
Addiction has a significant genetic component. Research suggests that genes account for 40–60% of a person’s vulnerability to addiction. If you have a close family member with addiction, your risk is higher—not because addiction is “inherited” like eye color, but because certain genetic variations affect how your brain responds to substances or rewards.
Biological factors include: differences in dopamine receptor density, metabolism rates, and baseline stress hormone levels. Some people naturally produce fewer endorphins or have more sensitive reward circuits, making them more susceptible. That said, genes are not destiny. Environment and personal choices still play enormous roles, and many people with family histories never develop addictions.
Environmental and Social Influences
Where and how you grow up matters enormously. Environmental risk factors include:
- Exposure to substance use at home – Parents or siblings who use
- Peer pressure – Social circles where drinking or drug use is normal
- Trauma or abuse – Physical, emotional, or sexual trauma
- Poverty or instability – Chronic stress and limited resources
- Easy access – Living where substances are readily available
- Cultural norms – Communities that celebrate heavy drinking or gambling
The earlier exposure happens, the greater the risk. A teenager who starts drinking is far more likely to develop alcohol addiction than someone who starts in their mid-twenties, because adolescent brains are still developing impulse control and reward processing.
Lifestyle and Habit Patterns
Daily routines and habits shape addiction risk. People who lack healthy coping mechanisms—exercise, social connection, creative outlets—are more vulnerable to turning toward addictive behaviors when stressed. Poor sleep, irregular eating, and chronic boredom also play roles.
Habit patterns that increase risk include: using substances to celebrate, to cope, or to socialize; associating specific places or times with use (e.g., “wine o’clock” every evening); and lacking structure in daily life. The good news is that just as habits create addiction, new habits can undo it. Building a healthy daily routine is a core part of natural recovery.
Effects of Addiction on Health and Life
Short-Term Effects
The immediate effects of addiction depend on the behavior or substance, but common short-term consequences include:
- Impaired judgment – Leading to risky decisions
- Mood changes – Euphoria followed by crash, or irritability
- Physical symptoms – Nausea, headache, racing heart, dizziness
- Relationship conflicts – Arguments with loved ones
- Financial strain – Impulsive spending or gambling losses
- Sleep disruption – Staying up too late or sleeping poorly
These effects might seem manageable at first. The problem is that short-term relief comes with a price, and the price increases with each repetition.
Long-Term Health Risks
Over months or years, addiction takes a devastating toll on physical health. Specific risks include:
- Substance addiction – Liver cirrhosis, lung cancer, heart disease, brain damage, infectious diseases (from needle sharing), and organ failure
- Behavioral addiction – Chronic back or neck pain (from screen use), obesity or malnutrition, type 2 diabetes, cardiovascular disease from inactivity
- All types – Weakened immune system, chronic fatigue, early aging, and increased risk of accidents or injuries
Brain changes also become more entrenched, affecting memory, attention, and emotional regulation. Some damage is reversible with sustained recovery; some is permanent.
Impact on Relationships and Career
Addiction is often called a “family disease” because it hurts everyone close to the person. Trust erodes as lies and broken promises accumulate. Partners may feel abandoned, children may feel confused or blame themselves, and friends may drift away. Financial problems from addiction—gambling losses, money spent on substances, job loss—create additional strain.
Career consequences include: absenteeism, poor performance, lateness, strained coworker relationships, and termination. Legal problems (DUIs, theft to support addiction) can create criminal records that limit future opportunities. The shame of these consequences often drives further addictive behavior, deepening the spiral. Recovery isn’t just about stopping the addiction—it’s about rebuilding what was lost.
Natural Ways to Overcome Addiction
Yoga and Meditation for Recovery
Yoga and meditation address addiction at multiple levels. Physically, yoga reduces stress hormones like cortisol, improves sleep, and helps the body repair from substance damage. Mentally, meditation trains attention and impulse control exactly the skills addiction weakens. Studies show that regular meditation increases gray matter in the prefrontal cortex, the brain’s self-control center.
Practical tips: Start with just five minutes of breath awareness daily. Notice cravings without acting on them just observe the urge as a passing wave. For yoga, gentle styles like Hatha or Restorative are ideal for early recovery. Many treatment centers now offer mindfulness-based relapse prevention (MBRP), which combines meditation with practical coping skills.
Diet and Natural Detox Methods
What you eat profoundly affects mood, energy, and cravings. Addiction depletes the body of essential nutrients, so rebuilding is key. Focus on:
- Protein-rich foods – Eggs, beans, fish (provide amino acids for neurotransmitter production)
- Complex carbohydrates – Oats, sweet potatoes, brown rice (steady blood sugar reduces mood swings)
- Healthy fats – Avocado, nuts, olive oil (support brain health)
- Hydration – Water flushes toxins and reduces cravings
Natural detox methods include increasing fiber (to bind and eliminate toxins), drinking herbal teas (milk thistle supports liver health), and sweating through exercise or sauna. Always consult a doctor before any detox, especially from alcohol or benzodiazepines, as withdrawal can be dangerous.
Herbal and Holistic Therapies
Several herbs show promise for supporting addiction recovery, though they should complement—not replace—medical care when needed:
- Ashwagandha – Reduces stress and cortisol
- Milk thistle – Supports liver regeneration after alcohol use
- Passionflower or chamomile – Eases anxiety and improves sleep
- L-theanine (from green tea) – Promotes calm focus
- N-acetylcysteine (NAC) – An amino acid supplement shown to reduce cravings for cocaine, marijuana, and gambling
Holistic therapies include: acupuncture (used effectively for opioid and nicotine withdrawal), massage therapy (reduces physical tension and promotes relaxation), and art or music therapy (provides emotional expression without substances).
Lifestyle Changes and Habit Control
Lasting recovery requires restructuring daily life. Key changes include:
- Identify triggers – Keep a log of what prompts cravings (time of day, people, places, emotions)
- Change your environment – Remove alcohol from home, install website blockers, avoid gambling venues
- Build new routines – Morning exercise instead of morning coffee run, evening hobby instead of evening drinking
- Find healthy rewards – A hot bath, a good book, time with a friend
- Exercise regularly – Boosts dopamine naturally, reduces stress, improves mood
- Prioritize sleep – Fatigue weakens impulse control
Habit control technique: Use the “delay rule.” When a craving hits, tell yourself you can give in after 15 minutes. Often, the urge passes. If not, delay another 15 minutes. This builds the muscle of riding out cravings without acting.
When to Seek Professional Help
Warning Signs of Severe Addiction
Natural methods work best for mild to moderate addiction or as part of a broader plan. Seek professional help immediately if you or a loved one experience:
- Inability to stop despite serious consequences (job loss, legal trouble, health crises)
- Severe withdrawal symptoms – Seizures, hallucinations, vomiting, dangerously high blood pressure
- Using in dangerous situations – Driving, operating machinery, caring for children
- Tolerance escalation – Needing increasingly more to get the same effect
- Loss of consciousness – Blackouts or passing out
- Suicidal thoughts – Feeling like there’s no way out
- Injection drug use – Higher risk of overdose and infections
If multiple warning signs are present, professional treatment—detox, counseling, medication—may be necessary for safety.
Importance of Medical and Psychological Support
Professional help isn’t a sign of failure; it’s a sign of wisdom. Medical support is essential for safe withdrawal from alcohol, benzodiazepines, or opioids, as complications can be fatal. Medications like naltrexone, buprenorphine, or disulfiram can reduce cravings and prevent relapse.
Psychological support options include:
- Cognitive-behavioral therapy (CBT) – Changes thought patterns that drive addiction
- Motivational interviewing – Builds internal desire to change
- Support groups – 12-step programs (AA, NA), SMART Recovery, or Refuge Recovery
- Intensive outpatient or residential treatment – For moderate to severe cases
The most effective approach often combines professional care with natural methods. A therapist can help you address underlying trauma while you practice meditation and change your diet. Recovery is not about choosing one path—it’s about using every tool available.
Conclusion
Addiction isn’t a lack of willpower it’s a brain condition that affects control, behavior, and decision-making. It can involve substances, behaviors, or even everyday habits, all driven by changes in the brain’s reward system. The good news: recovery is possible at any stage. Natural approaches like yoga, meditation, and healthy lifestyle changes can support healing, while professional care is essential for severe cases. Progress starts small—one step at a time and every effort toward recovery truly counts.
Read More: Naturopathy support for cancer treatment.
